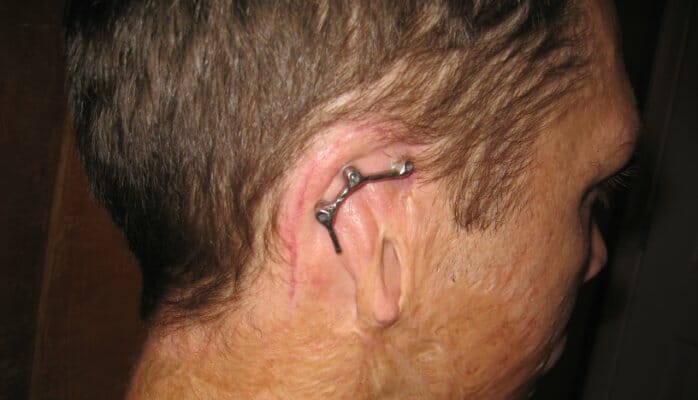
I have 3 screws permanently inserted into my skull. Some even say I have a few screws loose, which is not far from the truth. These screws were drilled into my head to secure my prosthetic ear, a dental implant technology that allows people such as myself to once again have matching ears. The process is quite involved, requiring 2 surgeries and 6 months of healing in between. I’ll spare you the details but essentially I now have 3 Frankenesque knobs sticking through my scalp, that in turn connect to a platinum bar for my prosthetic ear to snap onto. Basically, I’m a life size Mr. Potato Head. It’s not uncommon for my ear to pop off at the most inopportune time – especially while I’m dancing or playing with my kids at the playground. Sometimes it’s actually pretty cool walking around without the ear attached as I’m sure people are thinking it’s just a new piercing fashion. And when I need a good laugh, it’s fun to just leave my ear laying around in public places (gym locker room, hotel pillow – see pic below at Hartsfield Airport TSA screening). You may think that’s cruel but I think God gave me one ear for a reason… and that was to have fun and to show others how to be comfortable in their own skin.
If you can’t laugh at your own imperfections or deformities, life will be pretty miserable
Getting a prosthetic ear at the age of 36, especially after not having a right ear for 28 years, is quite an extensive process to get approved by a health insurer. Fortunately, I was able to work with an amazing doctor, Dr. Koenig, at BlueCross BlueShield of GA (BCBS) who deemed the procedure medically necessary and approved as “in network”. Once the procedure was approved in writing, I scheduled the initial implant surgery and verified with my employer multiple times they were not changing their coverage or carrier prior to my surgery. My surgery was scheduled on the 3rd of August and made sure our renewal on the 1st of August would not impact me. I’m sure our HR Director loved me calling/emailing her so much. Call me paranoid, but I’ve had some crazy stuff happen to me with my 35+ surgeries over the last 32 years. She verified our coverage was not changing so I went ahead with the surgery.
Surgery went great (pic above). I was back home that night resting in my own bed and prepared to be back at work the next day. With the 3 screws embedded in my skull, I was now on the surgery rotation to have the 2nd surgery 6 months later to complete the implant process (the six month period was to allow the implants to integrate with the skull – osseointegration). 7 days after the surgery – 10th of August, I received a letter from an insurance company (not BCBS) notifying me I was now an insured customer.
That’s odd I thought; I haven’t been notified by anyone and our policy renewal had already come and gone.
Interestingly, the letter was dated the 6th of August, 3 days after my surgery. I immediately called my HR director and was notified we had switched carriers. She informed me the decision was made on the 6th but the new carrier was made aware of my surgery on the 3rd. She also informed me it was not uncommon for policy renewal decisions to be made after the renewal date and then coverage backdated to the renewal date once the business terms were agreed upon. Not surprisingly, two weeks later I receive another letter from the new carrier informing me the screws in my head were not preauthorized, were out of network and not covered under my insurance. Shocker!
A messy situation
Tell me if my logic is crazy or was this truly mind blowing. My insurance plan renewed on the 1st and no change was made. I had surgery on the 3rd, old insurance still in effect. I left the hospital on the 3rd, old insurance still in effect. On the 6th, my employer changed health insurance carrier and coverage was backdated to the 1st, 2 days before my surgery. In short, I just had $10,000 of titanium screws permanently drilled into my skull that I had spent the last 6 months getting preapproved as “medical necessity” and now being told I’m financially liable for all the expenses. The new insurance carrier denied the surgery and deemed the procedure as being “out of network” and not a “medical necessity”. After extensive sit downs with my employer, they had the HR Director reach out to the carrier multiple times over the next 3 months. She continuously told me ”don’t worry about it, I’m sure they’ll do the right thing.”
Well guess what, they didn’t. After explaining to my surgeon’s office every month what was happening, the carrier communicated directly to their office via denial of benefits letter that the $10,000 medical bill was my responsibility and that the 2nd surgery would only be covered as “out of network” if their review panel deemed the procedure as medically necessary. All I could think was,
“You’re kidding me, right?“
I have 3 screws permanently attached to my skull and you’re telling me my surgeon has to prove the importance of completing the full procedure. Who in their right mind walks around with random screws sticking out of their head – ok, maybe Frankenstein, but at least he had super human strength. All I wanted was an ear.
Just to reiterate to make sure we’re all on the same page, the day of my surgery, all of my surgeries, as well as the actual prosthetic ear itself were preapproved as “in-network” and I had met my calendar year deductible. With the new carrier, who was selected after my surgery with the policy coverage backdated to before my surgery, I now was on the hook for $20,000 if I had the 2nd surgery and received the prosthetic ear (which I had already been casted for). Had I been told the surgery was not covered prior to getting the implants, I would have postponed the surgery and reviewed my options. With my back against the wall and my employer unwilling to apply leverage with the carrier, I called the Ga Insurance Commission and Department of Labor. I was told by both agencies that although the situation was unfortunate, there was nothing they could do and their advice was to get an attorney involved to see if the carrier’s posturing changed.
Taking matters into my own hands
Armed with their guidance, I sought the advice of my good friend David Decker, who also was an attorney (Decker Law Firm). As a courtesy to me and angered by the bullying of the carrier, he agreed to escalate the situation. David quickly drafted a letter to my employer and to the carrier, putting them all on notice about my situation and how steps for resolution needed to be reached very quickly. This is not the forum for a juicy back and forth legal showdown, but let’s just say it got very interesting… some people’s tempers flared while others recognized this was not personal and we needed to focus on resolving the issues. David is awesome because he is extremely practical and just focuses on amicable resolution (everyone puts a little skin in the game but everyone wins too). After 6 weeks of arm wrestling, the new carrier finally agreed to honor BCBS’s preauthorization and medical necessity determination once I paid my new deductible.
When the dust settled and everyone was paid, I had to come out of pocket an additional $3000 (including legal fees and a new deductible) for surgery I owed $0 when I left the hospital. It was not a perfect ending but was much better than paying $20,000 and at some point you just make the most of a bad situation and move on. I share this experience so others understand just how complicated health insurance can be and how an employer’s decision to switch carriers can have big impacts. Imagine how the surgeon felt. He did his job and did it well and now he was caught in the middle of this insurance showdown – special thanks to Dr. Glen Maron and his staff for their patience and diligence. I would never expect an employer not to switch carriers just because one employee had a unique situation. However, I would expect an employer that is aware of their employee’s situation to communicate what they’re doing and why. It’s amazing how something as simple as communicating can resolve so much. Please know I have no hard feelings towards the carrier or my past employer about this situation, never did. I realize crazy things happen but I expect people to own up to their mistakes or lack of foresight and use their best efforts to resolve the situation and not make excuses. Trust me, I’ve seen it all and you’ll read about more of this in the near future.
Lastly, special thank you to Dr. Koenig of BCBS who actually took the time to read my story and approve the procedure to give me a right ear and an even brighter perspective on life. I only wish he knew how grateful I am of his generosity and how much something as simple as an ear can change someone’s life. He truly made a difference in my life and gave me hope that most people in the health insurance business want to help others.
ABOUT SHAY
Shay is an All American and World ranked triathlete, burn survivor with scars over 65% of his body and is a sought out national motivational speaker. Despite being told he’d never compete in sports again at the age of 8, Shay is living testament to “Anything is Possible”: 4x Ironman, 4x member of Team USA, ranked top 1% of Ironmen worldwide and has competed in 9 triathlon world championships, including the Ironman World Championships in Kona, Hawaii. His mantra has always been to not merely be a “finisher” but to be a “competitor.” If you enjoyed this article, I encourage you to check out my other posts.